 Last summer, Patient Choices Vermont (PCV) proudly co-sponsored the opening of a new play titled Act 39, written by Rob Mermin, founder of Circus Smirkus. Act 39 received rave reviews and sold out every performance. Building on this success, Act 39 will return to the stage for performances in three Vermont locations during August and September this year. Click to get your tickets for Act 39:
PCV is delighted to once again co-sponsor this sensitive, insightful, and deeply moving piece of theater. We encourage you to join us for a dramatic exploration of a true experience with medical aid in dying. Additionally, we invite you to stay for conversations with PCV, the playwright, and the cast after selected shows . Watch the trailer from the 2023 performance of ACT 39: Special Thanks to Rita Mannebach and her Family:
We are grateful to share the poignant story of Rita Mannebach, published in Seven Days this week. Read the full article here. Rita traveled from her home in Florida to Vermont to experience the final days and exit she chose, touching the hearts of many during her brief stay. Her son, Mike, expressed his heartfelt gratitude in a reflection that resonates deeply: "I can't think of words big enough to express my gratitude ("thanks" is far too small!) for everything you did to enable my mom to leave this world peacefully, painlessly, fearlessly, on her own terms. As I'm starting to be able to reflect with a somewhat clearer head, I'm appreciating more and more what an enormous gift it was for her and for her family and friends. I know you know this already, but I'm going to say it anyway: your efforts make a huge difference, to real people, every day. Thank you for your efforts and perseverance from the bottom of my heart." — Mike Mannebach PCV Wayfinder Meg Tipper adds, “What a rare privilege it was to know Rita and to help her achieve the death she desired. Her passionate advocacy for death with dignity was evident in her decision to engage in this PR just days before her passing. I came to love her in the short time I knew her.” As a testament to her advocacy and kindness, Rita made a generous final donation to PCV, supporting our mission to empower individuals at the end of life. We extend our deepest sympathies and heartfelt thanks to her family. We also want to express our gratitude to all PCV supporters. Your donations and words of encouragement fuel the compassionate work carried out by our small staff and dedicated team of volunteers. Your contributions create a ripple effect throughout the community. Patient Choices Vermont (PCV) has taken an important step in supporting both patients and clinicians by publishing a standardized set of instructions for the use of medical aid in dying in Vermont.
Previously, patients and their caregivers have had to make extra calls to their doctors receive answers to common questions like:
"You’ve been so helpful. I’m so grateful that you called me back even on a Saturday. I’m just trying to arrange what my mother wants. I know the end is pretty soon, and it’s hard.” - PCV Helpline callerNavigating the end-of-life process can be incredibly challenging for patients and their loved ones. Evaluating all the options, including medical aid in dying, and tackling the necessary steps can feel daunting, even overwhelming. This is where our compassionate Helpline team steps in, offering knowledgeable and caring assistance to patients as well as their spouses, children, siblings, and friends.
“My family is grateful every day that Maggie’s death was like her life,
one of powerful personal choice.” ~ Katy Lesser We know from Vermont Department of Health data and from our own helpline experience, that the number of people who are considering or using medical aid in dying in Vermont has tripled over the past two years.
Big Step in New Hampshire | End of Life Options Act to be heard by House of Representatives3/12/2024
For the first time ever, a medical-aid-in-dying bill is making its way through the New Hampshire legislature. On Tuesday, the New Hampshire House Judiciary Committee voted 13-7 to recommend that HB1283, the NH End of Life Options Act, be heard by the full House of Representatives. A vote could happen as soon as two weeks from now.
A medical aid in dying law similar to Vermont’s Act 39 has been introduced in the New Hampshire legislature. A hearing is scheduled before the NH House Judiciary Committee on February 7.
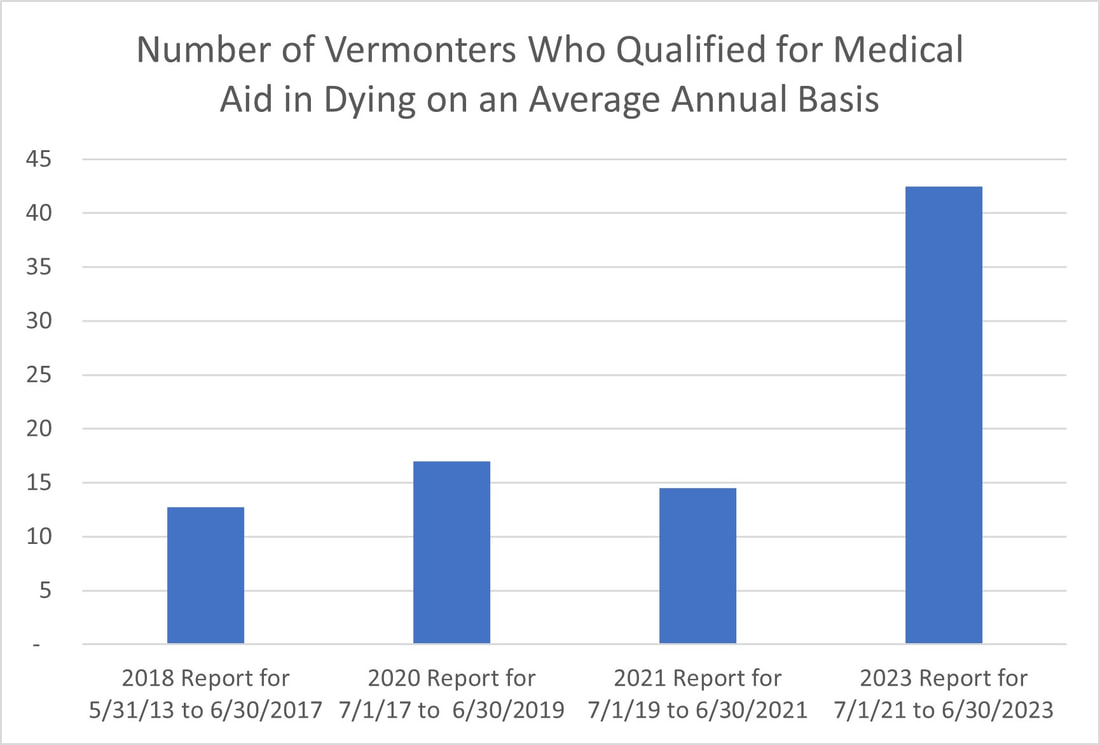
 “Medical aid and dying is so centrally important to my soul and to my peace of mind and to ending this one beautiful and amazing life the way I want it to end.” - Lynda Bluestein The Vermont Department of Health has just released its report on medical aid in dying for the period of July 1, 2021 to June 30, 2023. This bi-annual report offers statistics indicating that access to Medical Aid in Dying in Vermont has expanded in recent years.
 For the past five years, Patient Choices Vermont (PCV) has been fortunate to have retired nurse Toni Kaeding as one of our principal volunteers. As the main voice on our Helpline, Toni has offered more than 750 callers clear information, expert guidance, and a sympathetic ear. We are pleased to have recognized Toni’s outstanding work at a recent PCV board meeting. As a token of our appreciation for her many contributions, we sent Toni a pair of made-in-Vermont Darn Tough Socks. Profits from this special ‘Sweet as Syrup’ sock promotion provide meals to the Vermont Foodbank. |
Categories
All
Archives
July 2024
|
Proudly powered by Weebly



 RSS Feed
RSS Feed